Please watch our newest television ad. We are very proud to serve all our patients with providing the best healthcare available in Chicago!
Category Archives: CentMed News
Central Medical Clinic of Chicago offers Immigration Exams required by United States Citizenship and Immigration Services. Both, Dr. Anna Birn – Forys and Dr. Victor Forys are certified and authorized by USCIS to perform the exam as well to provide report on the exam. Please call us anytime at 773 545 2525. Also, please visit […]
What is the link between diabetes and heart disease? Having diabetes means that there is too much sugar (glucose) in your blood. If blood sugar stays high for a long time, the inner lining of blood vessels may be damaged. This makes it easier for cholesterol to build up, forming plaques in the walls of […]
What is a breast self-exam? A breast self-exam is an exam you can do yourself to check for breast cancer. When you do a breast self-exam, you check for lumps, thickening, and dimples in the breast. You also check for lumps in your underarms and discharge from the nipple.Ask your healthcare provider about doing breast […]
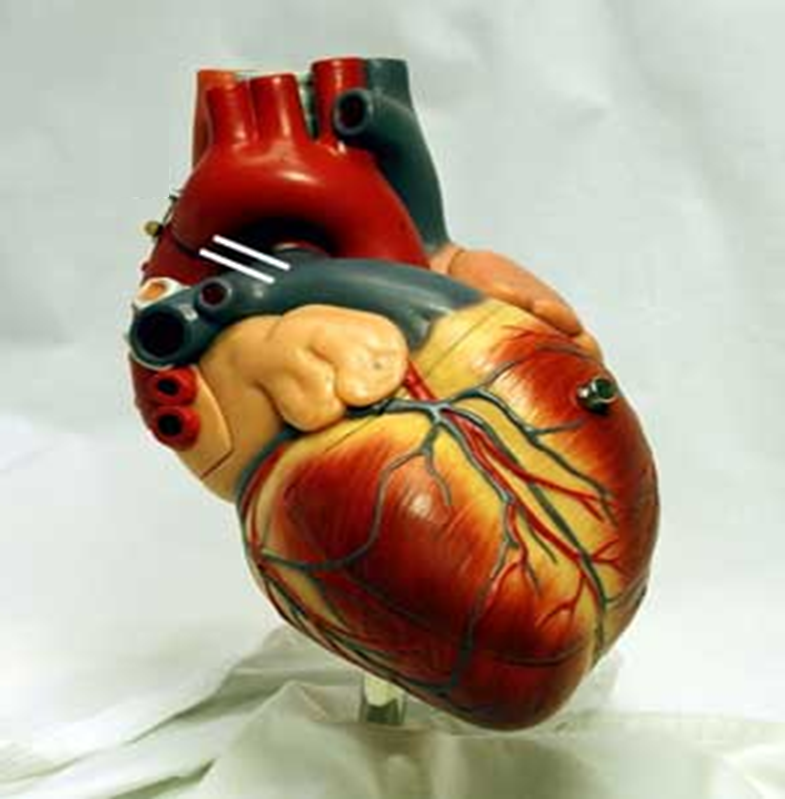
What is coronary artery disease? Coronary artery disease (CAD) is a type of heart disease. Your heart gets oxygen and nutrients from the blood that flows through the coronary arteries. When you have CAD, thick patches of fatty substances stick to the walls of the coronary arteries. These patches are called plaque. As the plaque […]
Prostate Cancer What is prostate cancer? Prostate cancer is the growth of abnormal cells in the prostate gland. The prostate gland is part of a man’s reproductive system. It is, on average, a little bigger than a walnut. It is located between the base of the bladder and the beginning of the penis. It surrounds […]
Mammogram What is a mammogram? A mammogram is a low-dose X-ray that examines breast tissue. When is it used? A mammogram helps detect breast cancer at an early stage. Mammograms can detect some types of cancer before you or your healthcare provider can feel a lump. They detect most cancerous growths in the breasts.Mammograms are […]
Asthma What is asthma? Asthma is a chronic (long-lasting) lung disease in which the lining of the airways of the lungs is often swollen or inflamed. Asthmatic airways are also unusually sensitive to certain irritants or “triggers.” An asthma trigger can be something your child is allergic to such as pollen, animal dander, or house […]
Pap Test What is a Pap test? A Pap test is a screening test done during a pelvic exam. It checks for abnormal changes in the cells of the cervix. The cervix is the lower part of the uterus that opens into the vagina. Abnormal cells can develop into cancer if they are not found […]
- 1
- 2